The OIG announced a new focused audit that will be conducted in FY 2023. The audit focuses on beneficiary eligibility for hospice services in the absence of a recent hospital encounter. How will your organization respond to this news?
Both the Centers for Medicare and Medicaid Services (CMS) and the Health and Human Services Office of Inspector General (OIG) are charged with preventing fraud and abuse related to federal healthcare spending. Audits and focused reviews are two of the tools used to identify instances of fraud and abuse and educate providers with a goal of minimizing further fraud and abuse in the future. Hospice industry leaders routinely find themselves responding to new or changing regulatory oversight.
The OIG announced a new focused audit that will be conducted in FY 2023. The audit focuses on beneficiary eligibility for hospice services in the absence of a recent hospital encounter. Questions about the audit abound and there are as many different responses to this news as there are different hospice organizations.
How will your organization respond to this news? Let’s explore how to respond to the new audit through the eyes of one CEO.
Michah’s Story Begins:
It is January 2022, and hospice agencies are still struggling to provide care in the midst of a pandemic. Everyone is doing the best they can with ever-shrinking resources. Michah, the CEO of a mid-size hospice, is reviewing hospice industry news update emails when he comes across the following announcement.
OIG Nationwide Review of Hospice Beneficiary Eligibility
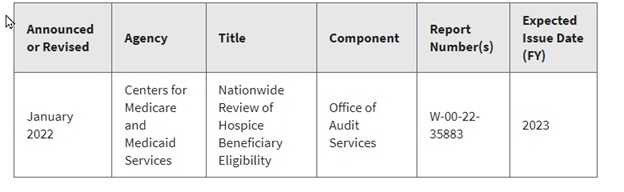
Michah reads further and learns that the Health and Human Services Office of Inspector General (OIG), is acting in response to compliance audits performed by the Office of Audit Services (OAS), which showed negative findings related to beneficiary eligibility. The OIG’s response is a nationwide review of hospice eligibility, focusing on patients admitted to hospice who have not had an inpatient or outpatient hospital encounter in “certain periods” prior to their hospice admission.
A Hospice CEO’s First Reactions
Michah is stunned! First, Michah works his way through the many three-letter abbreviations, ensuring he understands the players involved. These are Michah’s top concerns:
Why Did the OIG Pick this Topic?
Michah should take a deep breath and think through the focus of the audit. The OIG does not conduct random audits; there is a purpose behind each item on their work plan. Here are some facts that may explain why this item was added to their work plan:
Michah’s Gut Response to Mitigate Risk
Michah’s initial reaction is to slow admissions for patients who are not coming from the hospital, the type of patients which are the focus of the audit. The intake team will be instructed to gather data from other medical providers and present it to the hospice medical director for her review prior to scheduling an admission.
Michah is confident this approach will mitigate any risk.
A More Measured Response, by the Numbers
Michah’s gut response is not going to be helpful to his agency. Instead, Michah needs to understand his agency’s risk. This requires a close look at the agency’s data.
Michah now knows he has 348 patient admissions at risk for the OIG eligibility audit. The intake team data shows that it takes an average of 72 hours for referral information to be received once it is requested. Michah uses this data to evaluate the impact of his initial plan.
What Else Should Michah Consider?
Michah met with the agency’s performance improvement team to discuss the upcoming OIG audit. The team decided they needed to review and document the following data points prior to coming up with a plan to address their risks:
For more about documentation, check out our Successful Documentation series.
Preparing Together for Increased Oversight of Eligibility Documentation
Michah and the team worked together to begin outlining a plan to prepare the agency for increased oversight of eligibility documentation. The used these important points as a starting point for their planning.
An Opportunity for Immediate and Ongoing Improvement
Michah has a solid plan for success for his hospice agency. Michah knows October 1, 2022, will be here before he knows it—and that he and his team will be ready. They decide to:
Are You Prepared?
Have you taken any steps to prepare for the OIG eligibility review? Any steps beyond an initial panicked response?
Rest assured you are not alone. There is still time to respond with positive action. Gather your data, then build a plan that addresses your organization’s risks. Use your organization’s performance improvement process to strengthen your organization where needed. Consider Michah’s response and utilize the aspects that work for you!
If you want to learn more, check out our webinar, Prepping for Pending Audits: Hospice Eligibility in 2023. We’ll cover what you need to know about the audit, best practices to prepare, and industry tools that can help support your eligibility process.






